As a renal dietitian for over ten years, I have found that caring for people with kidney disease takes compassion, dedication, and a lot of good clinical judgment. I love renal nutrition because it is complex and evolving, and there are always opportunities to learn and grow.
As kidney-care dietitians, our priority is to keep patients healthy and safe but extends beyond monitoring electrolytes, MBD, and albumin. In addition, we aim to help people with CKD live longer, healthy lives using the power of nutrition.
A more recent discovery in renal nutrition is the role of the gut on kidney health and even the association with mortality. One of the things I've wanted to learn more about is how to leverage gut health to improve the health and longevity of CKD patients.
While not a common practice in Nephrology at this time, there is mounting evidence that targeting gut health with fiber, prebiotics, and probiotics is a promising therapeutic approach for managing and treating CKD.
Disclosure: This post is sponsored by Kibow Biotech, the producer of Kibow Fortis, a multistrain prebiotic created for kidney health. As always, all opinions are my own.

The Kidney-Gut Axis
Before diving into the specifics of how and when to utilize fiber and prebiotics in our patients with kidney disease, let's take a minute to review the kidney-gut axis. If you are already familiar with the kidney-gut axis, feel free to skip this overview. But if not, this is important to understand.
A review of the microbiome
The microbiome refers to the bacterial flora that naturally resides in our digestive tract. For decades researchers have been uncovering the role that the microbiome plays in human health and has found it to be a key player in numerous body functions, including:
- Immunity
- Inflammation
- Absorption and sythesis of certain nutrients
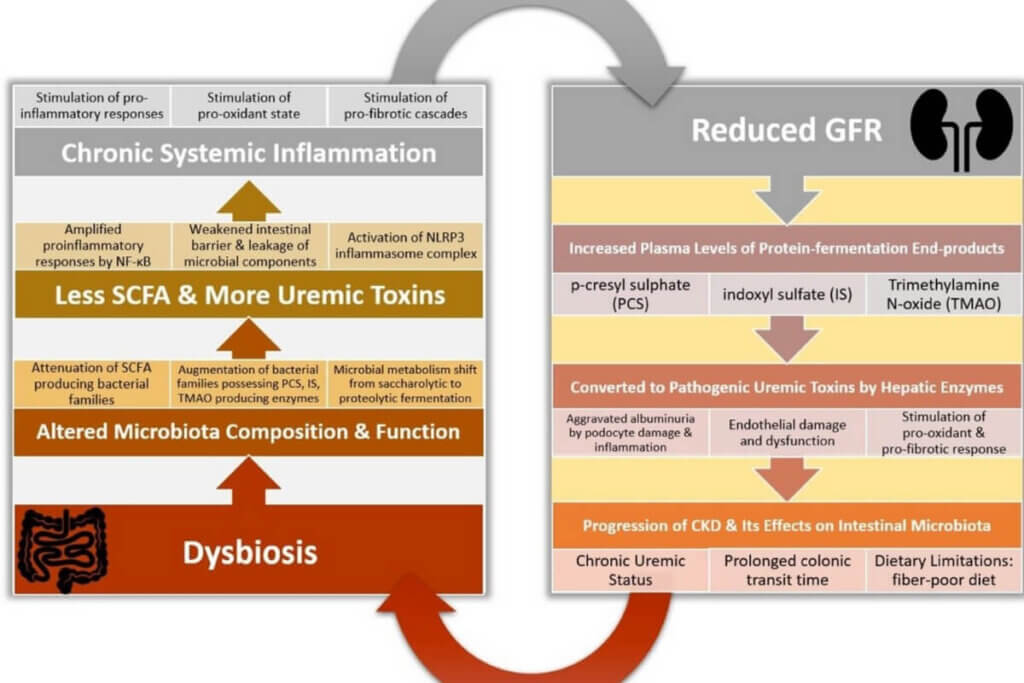
Dysbiosis occurs when the microbial population of the gut is imbalanced, and pathogenic and undesirable bacteria take over the beneficial bacteria. Dysbiosis is linked to a vast number of disease states, including CKD.
How are CKD and dysbiosis connected?
I often wonder if dysbiosis in CKD is a chicken or the egg type of scenario- which came first? So here is what we know so far about how dysbiosis and CKD are related.
1. Increased production of endotoxins and uremic toxins
With decreased kidney function, urea concentration in the blood and other fluids increases, including gastric juices. When urea enters the gut, it induces urease-containing bacteria to help break down urea into ammonia. These urease-containing bacteria can inhibit the growth of commensal bacteria, which can cause an excess of endotoxins and uremic toxins. (1)
2. Impaired protein metabolism
Studies show that protein metabolism is impaired in a uremic state. When undigested protein enters the colon, it is fermented by Proteolytic bacteria. The result is the production of the endotoxins known as p-cresol sulfate (PCS) and Indoxyl sulfate (IS). (2)
3. Weakened intestinal barrier and leaky gut
PCS and IS are known to degrade the epithelial lining of the intestinal lumen, allowing toxins from the gut to enter the bloodstream. These circulating toxins cause a cascade of inflammatory cytokines and are associated with the increased progression of CKD and increased risk of Cardiovascular disease (CVD). (3)
4. Chronic systemic inflammation
PCS and IS aren’t the only offenders known to affect the progression of both CVD and CKD. Trimethylamine N-oxide (TMAO), a toxic metabolite produced from the fermentation of choline and carnitine, triggers an inflammatory response and is a strong predictor of CVD and increased risk and progression of CKD. (4)
5. Inadequate fiber intake
Reduced fiber intake in patients with CKD (and, truly, the general population) is also a significant driver of dysbiosis. Fiber intake is typically inadequate on the Renal diet due to dietary restrictions. Lack of fiber causes a decrease in the beneficial saccharolytic bacteria (bacteria derived from carbs), short-chain fatty acid production (SCFA) like butyrate, and slow colonic transit time. (5)
Other factors that influence gut microbiota
Diet and uremia aren't the only causes of dysbiosis. We're all familiar with the unfortunate effects that medications like phosphorus binders (6), antibiotics, and even oral iron (7) can have on the gut.
Not only can they be a cause of GI side effects, but they can also wreak havoc on the gut's beneficial bacteria. While these are just a few examples, plenty of other medications may also alter normal gut bacteria.
Therapeutic opportunities for renal dietitians
Research over the past twenty years has shown a clear cause and effect between alterations in the microbiota and the progression and adverse outcomes in patients with CKD.
Now that we understand the why behind dysbiosis in CKD, studies are shifting to opportunities to use the gut to modulate the course of CKD, decrease uremic symptoms and inflammation, and improve cardiovascular outcomes. These opportunities present new therapeutic approaches to help patients live longer and healthier lives with CKD.
There are two primary areas of research of interest to renal dietitians:
- The use of fiber and prebiotics to increase the production of beneficial bacteria, short-chain fatty acids (for example, butyrate), and Vitamin K production.
- Targeted use of probiotics that help restore microbial balance and potentially inhibit the production of uremic toxins and toxic metabolites shows excellent promise in reducing inflammation, progression of CKD, and improved outcomes.
Because this is such a vast topic, for this post, we are covering fiber and prebiotics. Looking for information on probiotics? Check out our post A Renal Dietitians guide to probiotics and Kidney Disease!
Fiber

We all know the critical role that fiber plays in health. It's all about fiber from gut health, diabetes, cardiovascular disease, and even weight management! And while 25-35 grams per day is the general recommendation, data from the NHANESIII survey show that the average American's intake is only 16 grams per day.
What are the benefits of fiber specific to patients with CKD?
While fiber is beneficial to everyone, studies are showing that it is crucial for individuals with CKD. What stands out to me most about this is its simplicity. We can leverage the power of fiber through food or even supplements to enhance health! Here are just a handful of ways fiber can improve the health of kidney patients.
1. Decreased inflammation and mortality
In 2012, Krishnamurthy et al. looked at the data from the NHANES III survey to identify the association between fiber intake, inflammation, and all-cause mortality in individuals with CKD compared to those without CKD.
They found that higher fiber intake was associated with decreased incidence of inflammation in those with and without CKD. However, individuals with CKD who had a higher fiber intake showed lower overall mortality than the non-CKD subset. (8)
2. Decreased cardiovascular risk
Fiber intake is directly associated with cardiovascular disease- the leading cause of morbidity and mortality in patients with CKD. (9) And it's not just the traditional risk factors like hypertension or dyslipidemia that increase CV events. CV disease risk is also linked to the gut!
Remember the uremic toxin P-cresyl sulphate (PCS) and the toxic metabolite Trimethylamine N-oxide (TMAO)? TMAO and PCS are both correlated with worse cardiovascular outcomes and are associated with a lower fiber diet. (10), (11)
Using dietary fiber or fiber supplements is an important way to decrease cardiovascular disease!
3. Better blood sugar management
Fiber is a VIP when it comes to blood sugar management. (12) Blood sugar control is essential for patients in earlier stages of CKD because poor glucose control correlates with the faster progression of the disease. In addition, patients with CKD taking immunosuppressive medications or other medications that increase the risk of developing diabetes also benefit from increased fiber intake.
4. Increased bowel transit time
Raise your hand if you work with patients that complain of constipation? Are all hands up? Yep, we thought so! Unfortunately, constipation is a common complaint from people with CKD and is especially prevalent amongst those who require dialysis.
A whole slew of factors affects intestinal motility for people with CKD, including:
- Medications
- Inadequate dietary fiber
- Fluid restrictions
- Diabetes
Increasing fiber intake to the recommended 25-35 grams per day may help increase bowel transit time, alleviate constipation, and, as a bonus, potentially improve phosphorus and potassium levels. (13) Talk about a win-win!
5. Reduction in uremic toxins
In the most recent issue of the Journal of Renal Nutrition September 2021, Yang et al. conducted a meta-analysis that concluded that dietary fiber supplementation in patients with CKD significantly reduced PCS, IS, uric acid, and creatinine! (14) Holy smokes, this is a big deal and what's impressive about it is just how simple of a solution this is!
While there were no clear guidelines in the reviewed studies on how much additional fiber and what types of fiber supplement had the most benefit, the overarching theme is that higher fiber intake correlates with improved outcomes!
6. Nourishing the beneficial bacteria in the gut
Fiber-rich foods supply the beneficial bacteria "probiotics" with their preferred food source: undigestable carbohydrates, aka prebiotics. These beneficial bacteria, or super-heroes as we like to think of them, can increase SCFA production, specifically butyrate, which helps restore the integrity of the intestinal wall lining. (15)
From what we already know about the potential implications of dysbiosis, restoring the balance of the microbiota can profoundly impact the health and outcomes of patients with CKD.
Overcoming barriers to adequate fiber intake
We all know that most of our patients with CKD, just like many Americans, are not eating enough fiber. Whether that's due to potassium and phosphorus restrictions, accessibility to healthy plant foods, or dietary habits, the case for more fiber couldn't be more transparent!
CKD patients at all stages need adequate fiber for long-term health. Helping patients meet dietary fiber recommendations is an incredible opportunity for Renal Dietitians to help patients change their health and disease trajectory.
A food-first approach
Many patients have no problem meeting their fiber needs, especially when they are focused on eating plenty of fresh fruits and vegetables.
However, we know that this is not the case for all patients. So, how can we support individuals that are struggling to consume adequate fiber? Here are just a few strategies that may be helpful:
- Choose 2-3 vegetables to easily add to meals or snacks over the next week
- Use fresh or frozen fruit for dessert or snacks
- Swap a few favorite refined grain products for whole grains
- Add nuts or seeds as snacks or sprinkled on meals
- Try at least one or two meals per week that use beans or legumes
Helping patients find easy (and tasty ways) to add fiber-rich foods should be the first-line approach, but prebiotic fiber supplements can also be a helpful tool.
Prebiotics: The primary food source for probiotics

What are prebiotics?
Prebiotics was defined in 2008 by the 6th Meeting of the International Scientific Association of Probiotics and Prebiotics (ISAPP) as a "selectively fermented ingredient that results in specific changes in the composition and/or activity of the gastrointestinal microbiota, thus conferring benefit(s) upon host health." (16)
Prebiotics are found in non-digestible carbohydrates (fiber and resistant starch). However, there is evidence that prebiotics may also come from non-carbohydrate food sources such as polyphenols, PUFA's, and conjugated linoleic acids. (17)
The role of prebiotics in human health is currently a hot topic in research. Studies are looking to use prebiotics that targets specific bacterial strains that can modify different diseases and conditions, including CKD.
The benefit of prebiotics is that they provide constant and consistent fuel for the healthy bacteria in the gut but ensuring a diverse and varied diet to feed specific strains of bacteria can be a challenge.
Types of prebiotics
Fiber that meets the criteria for prebiotics include:
- Fructans (Fructo-oligosaccharides(FOS), Inulin, and oligosaccharides)
- Lactulose
- Soybean oligosaccharides
- Galactosaccharides (18)
Prebiotic fiber is present in a variety of fiber-rich plant foods. For instance, the list below consists of some of the most standout sources:
- Whole grains
- Beans
- Onions/garlic/ leeks
- Banana
- Asparagus
- The elusive Jerusalem artichokes (if anyone can actually find this let us know)
- Jicama
- Chicory root
Prebiotic supplements
With new interest and understanding of the importance of gut health for human health, the market for prebiotic fiber is booming!
You can find prebiotic supplements as isolated prebiotic fiber or combined with several prebiotic fibers in one product. They typically are found in tablet, capsule, or powder form.
In addition, you can find prebiotic fiber added to processed foods like protein bars, yogurts, and cereals. While fiber supplements aren't new, claims on the label that advertise them as a prebiotic source are becoming more common.

What are some examples of prebiotic fibers?
Research is emerging that targeted use of prebiotic fibers can have a positive effect on both gut health and CKD. Let's review the most popular fiber supplements available and any research to support their role in CKD.
The most commonly found fiber supplements available at retail stores likely have benefits but do not have much research to back them up:
Benefiber- wheat dextran
Metamucil -psyllium fiber
Fiber gummies- polydextran
The prebiotic fibers listed below have a great deal of research to support their use:
1. Multi-fiber prebiotics
Kibow Fortis is a unique and beneficial product that contains a mix of 7 different prebiotic fibers! Kibow Fortis includes both soluble and insoluble fiber and was uniquely designed to promote the beneficial bacteria lactobacilli and bifidobacteria.
The benefit of a multistrain prebiotic like Kibow Fortis is that it feeds various types of bacteria and can help support gut health for everyone, even those with an optimal diet.
To find out more about all of the different prebiotic fiber and their benefits, visit the Kibow Biotech website.
2. Acacia gum
Acacia gum also goes by the names "gum arabic or acacia Senegal." It has been studied extensively as a therapeutic prebiotic fiber for CKD. A study on mice with adenine-induced CKD showed that the addition of gum arabic decreased IS and caused restoration of intestinal dysbiosis by upregulating the number of beneficial bacteria and an increase in short-chain fatty acid production. (19)
3. SunFiber (guar gum or partially hydrolyzed guar gum)
A study conducted in mice with CKD found that the addition of guar gum(GG) and partially hydrolyzed guar gum(PHGG) reduced endotoxin production and increased Secretory IgA.
This study also found markers that suggest that GG and PHGG had a positive influence on colonic tight junctions improving the overall integrity of the gut. (20)
4. Inulin
Inulin can be found in both powder or tablet form and in addition, is commonly added to foods to increase fiber. A study by Lai et al. compared an LPD with LPD + inulin and found that the control group with inulin added showed a decrease in uric acid and C-reactive protein (CRP). (21)
5. Lactulose
I don't know about you, but I always considered lactulose to be a laxative. However, lactulose is a disaccharide and is found to have prebiotic powers promoting the growth of bifidobacterium and lactobacillus in lower doses. These two species of bacteria are known for their ability to produce SCFA's, especially butyrate. (22) SCFA's are well known to have a significant anti-inflammatory effect in the gut.
6. Resistant starches
Resistant starch cannot be completely broken down during the digestive process and acts as a prebiotic in the colon. So, where can you find resistant starch? Here are some of the familiar sources:
- Plantains
- Green banana
- Cooked and cooled rice, potato, and pasta
- Potato starch
- Beans
- Whole grains
Two common resistant starches used often are potato starch and green banana powder. They are becoming increasingly popular for diabetes thanks to their glucose-lowering effects. One of my clients swears by potato starch as her secret weapon to keep her blood sugar stable.
While there are not many studies in humans on the effects of resistant starch for CKD, several animal-based studies have shown promising results. Multiple studies have demonstrated that RS can cause an increase in beneficial bacteria that promotes the production of SCFA while also decreasing uremic toxins. We think that's pretty fantastic! (23)
7. Galactooligosaccharides
Bimuno is a brand that includes a line of prebiotic supplements containing galactooligosaccharides (GOS). GOS is derived from lactose and feeds bifidobacterium and lactobacillus- two essential bacteria for gut health.
The effect of GOS on the composition of gut microbiota and tubulointerstitial injury was evaluated in nephrectomized rats compared to a control group. The study results showed that the group of mice given GOS had lower serum IS and cecal indole concentrations.
Histological studies from this experiment also found that tubulointerstitial injury was lessened in the group given GOS compared to the control group without GOS. (24)

When to recommend a prebiotic supplement
We know that dietary fiber can offer incredible benefits naturally. Hence, the million-dollar question is when and why should we consider recommending a prebiotic fiber supplement to our patients over food?
One of the primary indications for recommending prebiotic fiber is when patients cannot consume adequate fiber or follow a low carbohydrate diet.
Another consideration for utilizing prebiotics is significant GI complaints, like gas, bloating, diarrhea, or constipation. These symptoms are a red flag that dysbiosis is present; therefore, restoring balance by providing fuel for beneficial bacteria is an essential first step!
Prebiotic fiber supplements are an inexpensive way to help modulate the gut and improve the health of our patients.
When patients with CKD implement aggressive dietary changes to delay or slow CKD progression, prebiotic therapy may be an adjuvant addition. While this is by no means a KDOQI guideline, it can undoubtedly be considered a "Won't hurt, might help" approach.
When would prebiotic fiber not be recommended?
One primary advantage mentioned before about fiber and prebiotics is that they offer a steady and consistent supply of preferred fuel for healthy bacteria. Although there are multiple benefits to adding more fiber and prebiotics into the diet, they may not be appropriate in all cases.
- Gastroparesis
Fiber delays gastric emptying, which can worsen symptoms of gastroparesis.
- Fluid restrictions
As we all know too well, it is vital to ensure adequate hydration to help move bulk through the colon when increasing fiber. However, increasing fluids isn't appropriate for all patients.
So how do we handle increasing fiber for folks on a tight fluid restriction? Utilizing resistant starch could be one way around this as it does to cause the bulking effect like soluble and insoluble fiber.
- IBS
For individuals with IBS that are following a low FODMAP diet, Fructans and GOS are well-known triggers. Foods rich in fructans and GOS include:
- Garlic and onions
- Legumes
- Many vegetables
- Grains
- Nuts/seeds
Two low FODMAP prebiotic fibers to consider for folks with IBS are SunFiber and Acacia gum.
Best practices for increasing dietary fiber and prebiotic supplements
Whether recommending an increase in dietary fiber or the addition of a prebiotic supplement, starting at a low dose and slowly titrating up is the best way to avoid GI upset.
While adding a prebiotic fiber, watch for GI complaints such as gas, bloating, constipation, and diarrhea. Scaling back on the dose or trying alternative options may be necessary for long-term success.
Supplementing with prebiotic fiber can be a temporary strategy while working with patients to increase dietary fiber. However, there is no substitute for the synergistic properties that whole food sources offer!
Final Thoughts
The connection between dysbiosis and kidney disease is clear, and research is now looking at ways to leverage gut health to improve the health and longevity of patients living with CKD.
Fiber and prebiotic supplements are key players in the health and wellbeing of everyone, including patients with CKD. When choosing a prebiotic supplement, considering an option that contains multiple prebiotic fibers can yield various benefits.
Kibow Fortis, a multistrain prebiotic, is a great option! Kibow biotech intentionally created this multi-beneficial product to treat dysbiosis, improve cholesterol and blood sugar management, enhance the immune system, and help with satiety and weight management.
Nutrition and gut health go hand in hand.
We all know the importance of a healthy diet that includes more plants, and we are over the moon excited to see that new research shows that there is a place for more plant foods for individuals with CKD. Not only is there a place, but recent evidence from research shows clear benefits!
It's time to shine, fellow renal dietitians! It's time to encourage our CKD community of what we've known all along, that fiber-rich foods fit in the renal diet!
Make sure to check out the second part of this series: A Renal Dietitian's Guide to Probiotics and Kidney Disease.
Interested in learning more about prebiotics and kidney care? Visit the Kibow Fortis website or Email to info@kibowbiotech.com